C1 Vertebral (Jefferson) Fracture
Summary:
-
A
C1 (atlas) vertebral fracture that usually occurs after an axial load injury
during a diving accident.
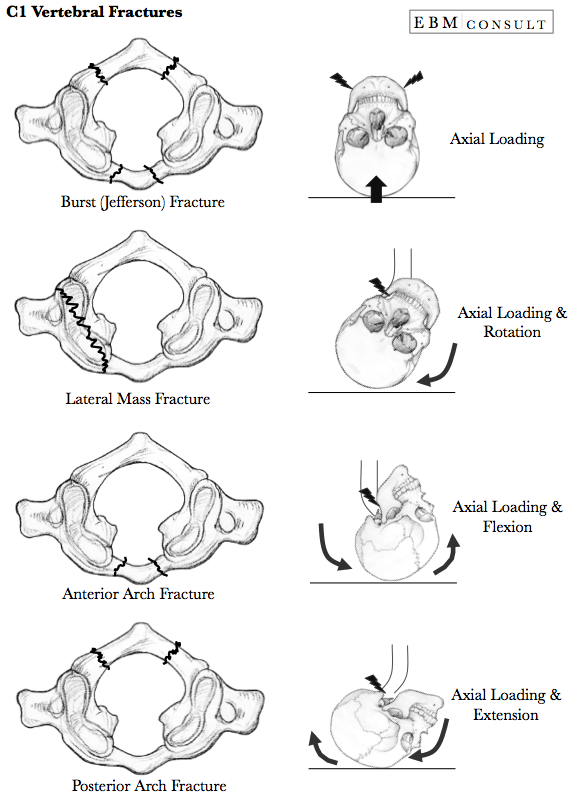
- When there are both anterior and posterior arch fractures this is called a "burst" fracture (also known as a Jefferson's fracture) and occurs when the occipital condyles are forced into the lateral masses of C1.
- While neurologic deficits may not always exist on presentation, imaging of the vertebral arteries is important due to concerns for late-onset neurologic deficits caused by blood flow disruptions.
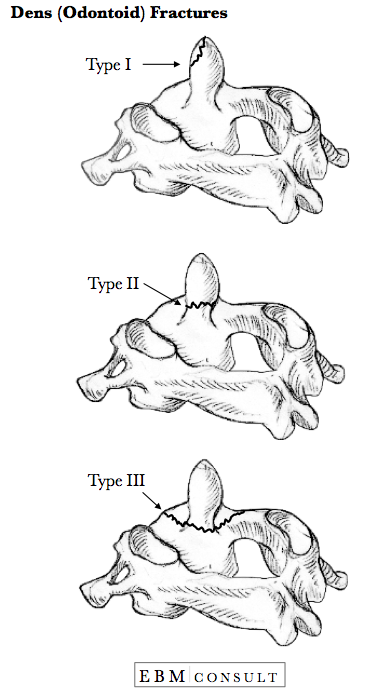
- There are 2 classifications for the different types of C1 fractures which are listed below.
C1 Vertebral Fractures
|
|---|