Tiagabine (Gabitril): Drug Monograph
|
|---|
- Treatment of partial seizures, as add on therapy in adults and children ≥12 years of age who are not controlled satisfactorily with other antiepileptic drug(s)
- Partial Seizures (Induced; Patients Already Taking Enzyme-Inducing Anticonvulsant Drugs):
- 4 mg by mouth once daily with food
- May increase total daily dose by 4 - 8 mg at weekly intervals until clinical response is achieved, or up to 56 mg/day, in divided doses (two to four times a day)
- Maintenance: 32 - 56 mg/day in divided doses (two to four times a day)
- Partial Seizures (Non-Induced):
- Requires lower dose and slower dose titration
- Partial seizures, 12-18 years, induced (patients already taking enzyme-inducing antiepilepsy drugs):
- 4 mg once daily
- May increase total daily dose by 4 mg at the beginning of Week 2, then by 4-8 mg at weekly intervals until clinical response is achieved, or up to 32 mg/day, in divided doses (two-four times a day)
- Refer to PI for typical dosing titration regimen
- Partial seizures, 12-18 years, non-induced:
- Requires lower dose and slower dose titration
- Impairment:
- May require reduced initial/maintenance doses and/or longer dosing intervals
- Known hypersensitivity to tiagabine or any of the tablet components
- Severely impaired liver function
- Follow recommended rate of dosage titration to minimize the potential for adverse events from a too rapid increment in dosage during the titration period.
- Risk of aggravation of absences in patients with generalized epilepsy
- Increase in seizure frequency or the onset of new types of seizures
- Non-convulsive status epilepticus (paradoxical)
- Generalized anxiety and depression
- Suicidal behavior and ideation
- Visual field defects
- Spontaneous bruising
- Serious rash, including vesiculobullous rash
- New onset seizures and status epilepticus in patients without epilepsy.
- Impaired hepatic function
- Dizziness
- Tiredness
- Somnolence
- Unspecific nervousness
- Tremor
- Diarrhea
- Abdominal pain
- Difficulty with concentration/attention
- Insomnia
- Confusion
- Pharyngitis
- Rash
- Depressed mood
- Emotional lability
- Somnolence, impaired consciousness, agitation confusion, speech difficulty, hostility, depression, weakness, myoclonus, seizures, respiratory arrest, non-convulsive status epilepticus, coma, ataxia, encephalopathy, amnesia, dyskinesia, drowsiness, headache, psychotic disorder, lethargy, spike wave stupor, tremors, vomiting, temporary paralysis and urinary incontinence may result.
- Activated charcoal may be used.
- Dialysis is unlikely to be beneficial.
- Antiepileptic drugs which induce hepatic enzymes (e.g., phenytoin, carbamazepine, phenobarbitone, and primidone) enhance the metabolism of tiagabine.
- Tiagabine is 96% bound to human plasma protein - has the potential to interact with other highly protein bound compounds.
- Pregnancy: Pregnancy Category C
- Labor and Delivery: None
- Nursing Mothers: Use with caution - weigh potential benefits vs possible risks
- Renal Impairment: None
- Hepatic Impairment: Adjust dosage by reducing the individual doses and/or prolonging the dose interval. Tiagabine is metabolized in the liver.
- Pediatric Patients: Safety and effectiveness in children below the age of 12 years have not been established.
- Geriatric Patients: Use with caution.
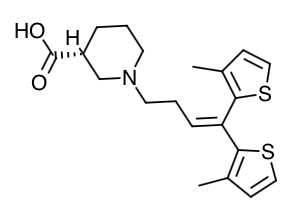
- Scientific Name: (-)-(R)-l-[4,4-Bis(3-methyl-2-thienyl)-3-butenyljnipecotic acid hydrochloride
- Empirical Formula: C20H25NO2S2
- Molecular Weight: 412.0
- The precise mechanism by which tiagabine exerts its antiseizure effect is unknown, although it is believed to be related to its ability, documented in in vitro experiments, to enhance the activity of gamma aminobutyric acid (GABA), the major inhibitory neurotransmitter in the central nervous system. These experiments have shown that tiagabine binds to recognition sites associated with the GABA uptake carrier. It is thought that, by this action, tiagabine blocks GABA uptake into presynaptic neurons, permitting more GABA to be available for receptor binding on the surfaces of post-synaptic cells. Inhibition of GABA uptake has been shown for synaptosomes, neuronal cell cultures, and glial cell cultures. In rat-derived hippocampal slices, tiagabine has been shown to prolong GABA-mediated inhibitory post-synaptic potentials. Tiagabine increases the amount of GABA available in the extracellular space of the globus pallidus, ventral palladum, and substantia nigra in rats at the ED50 and ED85 doses for inhibition of pentylenetetrazol (PTZ)- induced tonic seizures. This suggests that tiagabine prevents the propagation of neural impulses that contribute to seizures by a GABA-ergic action.
- Tiagabine has shown efficacy in several animal models of seizures. It is effective against the tonic phase of subcutaneous PTZ-induced seizures in mice and rats, seizures induced by the proconvulsant DMCM in mice, audiogenic seizures in genetically epilepsy-prone rats (GEPR), and amygdala-kindled seizures in rats. Tiagabine has little efficacy against maximal electroshock seizures in rats and is only partially effective against subcutaneous PTZ-induced clonic seizures in mice, picrotoxin-induced tonic seizures in the mouse, bicuculline-induced seizures in the rat, and photic seizures in photosensitive baboons. Tiagabine produces a biphasic dose-response curve against PTZ- and DMCM-induced convulsions, with attenuated effectiveness at higher doses.
- Based on in vitro binding studies, tiagabine does not significantly inhibit the uptake of dopamine, norepinephrine, serotonin, glutamate, or choline and shows little or no binding to dopamine Dl and D2, muscarinic, serotonin 5HT1A,5HT2, and 5HT3, beta-1 and 2 adrenergic, alpha-1 and alpha-2 adrenergic, histamine H2 and H3, adenosine A1 and A2, opiate µ and K1, NMDA glutamate, and GABAA receptors at 100 µM. It also lacks significant affinity for sodium or calcium channels. Tiagabine binds to histamine H1, serotonin 5HT1B, benzodiazepine, and chloride channel receptors at concentrations 20 to 400 times those inhibiting the uptake of GABA.
- Absorption: Absorption of tiagabine is rapid, with peak plasma concentrations occurring at approximately 45 minutes following an oral dose in the fasting state. Tiagabine is nearly completely absorbed ( > 95%), with an absolute oral bioavailability of about 90%. A high fat meal decreases the rate (mean Tmax was prolonged to 2.5 hours, and mean Cmax was reduced by about 40%) but not the extent (AUC) of tiagabine absorption. In all clinical trials, tiagabine was given with meals. The pharmacokinetics of tiagabine are linear over the single dose range of 2 to 24 mg. Following multiple dosing, steady state is achieved within 2 days
- Distribution: Tiagabine is 96% bound to human plasma proteins, mainly to serum albumin and al-acid glycoprotein over the concentration range of 10 ng/mL to 10,000 ng/mL. While the relationship between tiagabine plasma concentrations and clinical response is not currently understood, trough plasma concentrations observed in controlled clinical trials at doses from 30 to 56 mg/day ranged from < 1 ng/mL to 234 ng/mL.
- Metabolism: Although the metabolism of tiagabine has not been fully elucidated, in vivo and in vitro studies suggest that at least two metabolic pathways for tiagabine have been identified in humans: 1) thiophene ring oxidation leading to the formation of 5-oxo-tiagabine; and 2) glucuronidation. The 5-oxo-tiagabine metabolite does not contribute to the pharmacologic activity of tiagabine. Based on in vitro data, tiagabine is likely to be metabolized primarily by the 3 A isoform subfamily of hepatic cytochrome P450 (CYP 3 A), although contributions to the metabolism of tiagabine from CYP 1A2, CYP 2D6 or CYP 2C19 have not been excluded.
- Elimination: Approximately 2% of an oral dose of tiagabine is excreted unchanged, with 25% and 63% of the remaining dose excreted into the urine and feces, respectively, primarily as metabolites, at least 2 of which have not been identified. The mean systemic plasma clearance is 109 mL/min (CV = 23%) and the average elimination half-life for tiagabine in healthy subjects ranged from 7 to 9 hours. The elimination half-life decreased by 50 to 65% in hepatic enzyme-induced patients with epilepsy compared to uninduced patients with epilepsy.
- A diurnal effect on the pharmacokinetics of tiagabine was observed. Mean steady-state Cmin values were 40% lower in the evening than in the morning. Tiagabine steady-state AUC values were also found to be 15% lower following the evening tiagabine dose compared to the AUC following the morning dose.
- Special Populations:
- Renal Insufficiency: The pharmacokinetics of total and unbound tiagabine were similar in subjects with normal renal function (creatinine clearance > 80 mL/min) and in subjects with mild (creatinine clearance 40 to 80 mL/min), moderate (creatinine clearance 20 to 39 mL/min), or severe (creatinine clearance 5 to 19 mL/min) renal impairment. The pharmacokinetics of total and unbound tiagabine were also unaffected in subjects with renal failure requiring hemodialysis.
- Hepatic Insufficiency: In patients with moderate hepatic impairment (Child-Pugh Class B), clearance of unbound tiagabine was reduced by about 60%. Patients with impaired liver function may require reduced initial and maintenance doses of tiagabine and/or longer dosing intervals compared to patients with normal hepatic function.
- Geriatric: The pharmacokinetic profile of tiagabine was similar in healthy elderly and healthy young adults.
- Pediatric: Tiagabine has not been investigated in adequate and well-controlled clinical trials in patients below the age of 12. The apparent clearance and volume of distribution of tiagabine per unit body surface area or per kg were fairly similar in 25 children (age: 3 to 10 years) and in adults taking enzyme-inducing antiepilepsy drugs ([AEDs] e.g., carbamazepine or phenytoin). In children who were taking a non-inducing AED (e.g., valproate), the clearance of tiagabine based upon body weight and body surface area was 2 and 1.5-fold higher, respectively, than in non-induced adults with epilepsy.
- Gender, Race and Cigarette Smoking: No specific pharmacokinetic studies were conducted to investigate the effect of gender, race and cigarette smoking on the disposition of tiagabine. Retrospective pharmacokinetic analyses, however, suggest that there is no clinically important difference between the clearance of tiagabine in males and females, when adjusted for body weight. Population pharmacokinetic analyses indicated that tiagabine clearance values were not significantly different in Caucasian (N=463), Black (N=23), or Hispanic (N=17) patients with epilepsy, and that tiagabine clearance values were not significantly affected by tobacco use.
- Interactions with other Antiepilepsy Drugs: The clearance of tiagabine is affected by the co-administration of hepatic enzyme-inducing antiepilepsy drugs. Tiagabine is eliminated more rapidly in patients who have been taking hepatic enzyme-inducing drugs, e.g., carbamazepine, phenytoin, primidone and phenobarbital than in patients not receiving such treatment.
- Advise patients, caregivers, and families about increased risk of suicidal thoughts and behavior and to be alert for the emergence or worsening of symptoms of depression, any unusual changes in mood or behavior or emergence of suicidal thoughts, behaviors, or thoughts of self-harm. Instruct to report any behaviors of concern immediately to healthcare providers.
- Inform patients that dizziness, somnolence, and other symptoms/signs of CNS depression may occur; caution should be shown when driving or operating machinery while on treatment until adjusted to effects.
- Instruct patients to notify physician if pregnant, intending to become pregnant, or if breastfeeding. Encourage pregnant patients to enroll in North American Antiepileptic Drug Pregnancy Registry.
- If multiple doses are missed, instruct patient to contact physician for possible retitration.
Indications
Dosing (Adult)
General Dosing & Administration Notes: Take with food
Dosing (Pediatric)
Hepatic Dosing
Contraindications
Warnings
Adverse Reactions
Overdose
Drug Interactions
Special Populations
Chemical Structure
Mechanism of Action
Pharmacokinetics
Counseling Points
MESH Terms & Keywords
|
|---|
|





