Telavancin (Vibativ): Drug Monograph
|
|---|
- Treatment of adults with complicated skin and skin structure infections (cSSSIs) caused by susceptible gram-positive microorganisms
- Treatment of adults with hospital-acquired/ventilator-associated bacterial pneumonia (HABP/VABP) caused by susceptible isolates of Staphylococcus aureus (including methicillin-susceptible and -resistant isolates)
- Skin and skin structure infections:
- 10 mg/kg IV over 60 minutes every 24 hours for 7 -14 days
- HABP/VABP:
- 10 mg/kg IV over 60 minutes every 24 hours for 7-21 days
-
CrCl >50 mL/min:
-
10 mg/kg every 24 hours
-
CrCl 30-50 mL/min:
-
7.5 mg/kg every 24 hours
- CrCl 10-<30 mL/min:
- 10 mg/kg every 48 hours
- Insufficient data are available to make a dosing recommendation for patients with CrCl <10 mL/min, including patients on hemodialysis
- Patients with pre-existing moderate/severe renal impairment (CrCl ≤50 mL/min) who were treated with telavancin for hospital- acquired bacterial pneumonia/ventilator-associated bacterial pneumonia had increased mortality observed versus vancomycin. Use of telavancin in patients with pre-existing moderate/severe renal impairment (CrCl ≤50 mL/min) should be considered only when the anticipated benefit to the patient outweighs the potential risk.
- Nephrotoxicity: New onset or worsening renal impairment has occurred. Monitor renal function in all patients.
- Women of childbearing potential should have a serum pregnancy test prior to administration of telavancin.
- Avoid use of telavancin during pregnancy unless potential benefit to the patient outweighs potential risk to the fetus.
- Adverse developmental outcomes observed in 3 animal species at clinically relevant doses raise concerns about potential adverse developmental outcomes in humans.
- Decreased efficacy among patients treated for skin and skin structure infections with moderate/severe pre-existing renal impairment. Consider these data when selecting antibacterial therapy for patients with baseline CrCl ≤50 mL/min.
- Pregnancy women and women of childbearing potential - avoid use. Women of childbearing potential should have a serum pregnancy test prior to administration of telavancin.
- Hypersensitivity reactions - including anaphylactic reactions, may occur after first or subsequent doses. Use with caution in patients with known hypersensitivity to vancomycin.
- Infusion-related reactions
- Clostridium difficile-associated disease - may range from mild diarrhea to fatal colitis. Evaluate if diarrhea occurs.
- Development of drug-resistant bacteria
- QTc prolongation
- Coagulation test interference - including prothrombin time, international normalized ratio, and activated partial thromboplastin time.
- Discontinue telavancin and use supportive care with maintenance of glomerular filtration and careful monitoring of renal function.
- No information is available on the use of hemodialysis to treat an overdosage.
- The use of continuous venovenous hemofiltration (CVVH) is unknown.
- Drug-laboratory test interactions - telavancin interferes with the ability of the coagulation complexes to assemble on the surface of the phospholipids and promote clotting in vitro.
- Urine protein tests - telavancin interferes with urine qualitative dipstick protein assays, as well as quantitative dye methods
- Pregnancy: Pregnancy Category C
- Labor and Delivery: None
- Nursing Mothers: It is not known whether telavancin is excreted in human milk. Caution should be exercised.
- Renal Impairment: Higher incidence of renal adverse events in patients with underlying renal dysfunction or risk factors for renal dysfunction. Moderate/severe impairment: use should b e considered only when the anticipated benefit to the patient outweighs the potential risk. Dosage adjustment is required in patients with ≤50 mL/min renal impairment. Monitor serum creatinine closely and if renal toxicity is suspected, consider an alternative agent.
- Hepatic Impairment: No dosage adjustment is recommended with mild or moderate impairment.
- Pediatric Patients: Safety and efficacy not demonstrated.
- Geriatric Patients: Dosage adjustment for elderly patients should be based on renal function.
- It is not known whether telavancin is excreted in human milk. Caution should be exercised.
- Scientific Name: vancomycin,N3''-[2-(decylamino)ethyl]-29-[[(phosphono-methyl)-amino]-methyl]- hydrochloride
- Empirical Formula: C80H106Cl2N11O27P.xHCl (where x = 1 to 3)
- Molecular Weight: 1755.6
- The antimicrobial activity of telavancin appears to best correlate with the ratio of area under the concentration-time curve to minimum inhibitory concentration (AUC/MIC) for Staphylococcus aureus based on animal models of infection. Exposure-response analyses of the clinical trials support the dose of 10 mg/kg every 24 hours.
- Cardiac Electrophysiology: The effect of telavancin on cardiac repolarization was assessed in a randomized, double blind, multiple-dose, positive-controlled, and placebo-controlled, parallel study (n=160). Healthy subjects received telavancin 7.5 mg/kg, telavancin 15 mg/kg, positive control, or placebo infused over 60 minutes once daily for 3 days. Based on interpolation of the data from telavancin 7.5 mg/kg and 15 mg/kg, the mean maximum baseline-corrected, placebo- corrected QTc prolongation at the end of infusion was estimated to be 12-15 msec for telavancin 10 mg/kg and 22 msec for the positive control. By 1 hour after infusion the maximum QTc prolongation was 6-9 msec for telavancin and 15 msec for the positive control. ECGs were performed prior to and during the treatment period in patients receiving telavancin 10 mg/kg in 3 cSSSI studies to monitor QTc intervals. In these trials, 214 of 1029 (21%) patients allocated to treatment with telavancin and 164 of 1033 (16%) allocated to vancomycin received concomitant medications known to prolong the QTc interval and known to be associated with definite or possible risk of torsades de pointes. The incidence of QTc prolongation >60 msec was 1.5% (15 patients) in the telavancin group and 0.6% (6 patients) in the vancomycin group. Nine of the 15 telavancin patients received concomitant medications known to prolong the QTc interval and definitely or possibly associated with a risk of torsades de pointes, compared with 1 of the 6 patients who received vancomycin. A similar number of patients in each treatment group (<1%) who did not receive a concomitant medication known to prolong the QTc interval experienced a prolongation >60 msec from baseline. In a separate analysis, 1 patient in the telavancin group and 2 patients in the vancomycin group experienced QTc >500 msec. No cardiac adverse events were ascribed to prolongation of the QTc interval. In the Phase 3 HABP/VABP studies, the incidence of QTc prolongation >60 msec or mean value >500 msec was 8% (52 patients) in the telavancin group and 7% (48 patients) in the vancomycin group.
- Absorption: (Multiple dose) Cmax =1-8 mcg/mL, Auc0-24 = 780 mcghr/mL
- Distribution: Telavancin binds to human plasma proteins, primarily to serum albumin, in a concentration-independent manner. The mean binding is approximately 90% and is not affected by renal or hepatic impairment. Concentrations of telavancin in pulmonary epithelial lining fluid (ELF) and alveolar macrophages (AM) were measured through collection of bronchoalveolar lavage fluid at various times following administration of telavancin 10 mg/kg once daily for 3 days to healthy adults. Telavancin concentrations in ELF and AM exceeded the MIC90 for S. aureus (0.5 mcg/mL) for at least 24 hours following dosing. Concentrations of telavancin in skin blister fluid were 40% of those in plasma (AUC 0-24hr ratio) after 3 daily doses of 7.5 mg/kg telavancin in healthy young adults.
- Metabolism: No metabolites of telavancin were detected in in vitro studies using human liver microsomes, liver slices, hepatocytes, and kidney S9 fraction. None of the following recombinant CYP 450 isoforms were shown to metabolize telavancin in human liver microsomes: CYP 1A2, 2C9, 2C19, 2D6, 3A4, 3A5, 4A11. The clearance of telavancin is not expected to be altered by inhibitors of any of these enzymes. In a mass balance study in male subjects using radiolabeled telavancin, 3 hydroxylated metabolites were identified with the predominant metabolite (THRX-651540) accounting for <10% of the radioactivity in urine and <2% of the radioactivity in plasma. The metabolic pathway for telavancin has not been identified.
- Elimination: Telavancin is primarily eliminated by the kidney. In a mass balance study, approximately 76% of the administered dose was recovered from urine and <1% of the dose was recovered from feces (collected up to 216 hours) based on total radioactivity.
- Specific Populations
- Geriatric Patients: The impact of age on the pharmacokinetics of telavancin was evaluated in healthy young (range 21-42 years) and elderly (range 65-83 years) subjects. The mean CrCl of elderly subjects was 66 mL/min. Age alone did not have a clinically meaningful impact on the pharmacokinetics of telavancin.
- Pediatric Patients: The pharmacokinetics of telavancin in patients less than 18 years of age have not been studied.
- Gender: The impact of gender on the pharmacokinetics of telavancin was evaluated in healthy male (n=8) and female (n=8) subjects. The pharmacokinetics of telavancin were similar in males and females. No dosage adjustment is recommended based on gender.
- Renal Impairment: The pharmacokinetics of telavancin were evaluated in subjects with normal renal function and subjects with varying degrees of renal impairment following administration of a single dose of telavancin 7.5 mg/kg (n=28). The mean AUC 0∞ values were approximately 13%, 29%, and 118% higher for subjects with CrCl >50 to 80 mL/min, CrCl 30 to 50 mL/min, and CrCl <30 mL/min, respectively, compared with subjects with normal renal function. Dosage adjustment is required in patients with CrCl ≤50 mL/min. Following administration of a single dose of telavancin 7.5 mg/kg to subjects with end-stage renal disease, approximately 5.9% of the administered dose of telavancin was recovered in the dialysate following 4 hours of hemodialysis. The effects of peritoneal dialysis have not been studied. Following a single intravenous dose of telavancin 7.5 mg/kg, the clearance of hydroxypropyl- beta-cyclodextrin was reduced in subjects with renal impairment, resulting in a higher exposure to hydroxypropyl-beta-cyclodextrin. In subjects with mild, moderate, and severe renal impairment, the mean clearance values were 38%, 59%, and 82% lower, respectively, compared with subjects with normal renal function. Multiple infusions of telavancin may result in accumulation of hydroxypropyl-beta-cyclodextrin.
- Hepatic Impairment: The pharmacokinetics of telavancin were not altered in subjects with moderate hepatic impairment (n= 8, Child-Pugh B) compared with healthy subjects with normal hepatic function matched for gender, age, and weight. The pharmacokinetics of telavancin have not been evaluated in patients with severe hepatic impairment (Child-Pugh C).
- Drug Interactions
- In Vitro: The inhibitory activity of telavancin against the following CYP 450 enzymes was evaluated in human liver microsomes: CYP 1A2, 2C9, 2C19, 2D6, and 3A4/5. Telavancin inhibited CYP 3A4/5 at potentially clinically relevant concentrations. Upon further evaluation in a Phase 1 clinical trial, telavancin was found not to inhibit the metabolism of midazolam, a sensitive CYP3A substrate (see below).
- Midazolam: The impact of telavancin on the pharmacokinetics of midazolam (CYP 3A4/5 substrate) was evaluated in 16 healthy adult subjects following administration of a single dose of telavancin 10 mg/kg, intravenous midazolam 1 mg, and both. The results showed that telavancin had no impact on the pharmacokinetics of midazolam and midazolam had no effect on the pharmacokinetics of telavancin.
- Aztreonam: The impact of telavancin on the pharmacokinetics of aztreonam was evaluated in 11 healthy adult subjects following administration of a single dose of telavancin 10 mg/kg, aztreonam 2 g and both. Telavancin had no impact on the pharmacokinetics of aztreonam and aztreonam had no effect on the pharmacokinetics of telavancin. No dosage adjustment of telavancin or aztreonam is recommended when both drugs are coadministered.
- Piperacillin-tazobactam: The impact of telavancin on the pharmacokinetics of piperacillin-tazobactam was evaluated in 12 healthy adult subjects following administration of a single dose of telavancin 10 mg/kg, piperacillin-tazobactam 4.5 g, and both. Telavancin had no impact on the pharmacokinetics of piperacillin-tazobactam and piperacillin-tazobactam had no effect on the pharmacokinetics of telavancin. No dosage adjustment of telavancin or piperacillin-tazobactam is recommended when both drugs are coadministered.
- Women of childbearing potential (those who have not had: complete absence of menses for at least 24 months or medically confirmed menopause, medically confirmed primary ovarian failure a history of hysterectomy, bilateral oophorectomy, or tubal ligation) should:
- Be informed about the potential risk of fetal harm if telavancin is used during pregnancy.
- Have a pregnancy test prior to administration of telavancin.
- If not pregnancy, use effective contraceptive methods to prevent pregnancy during treatment.
- Notify their prescribing physician/ health care provider if they become pregnant during treatment.
- Patients should be informed that diarrhea is a common problem caused by antibiotics that usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as 2 or more months after having received the last dose of the antibiotic. Patients should be advised to contact their physician as soon as possible if this occurs.
- Patients should be counseled that telavancin should only be used to treat bacterial infections. Advise patients to take the medication exactly as directed. Skipping doses or not completing the full course of therapy may decrease the effectiveness of immediate treatment and increase the likelihood that the bacteria will develop resistance and will not be treatable by telavancin or other antibacterial drugs in the future.
- Patients should be informed about the common adverse effects of telavancin including diarrhea, taste disturbance, nausea, vomiting, headache, and foamy urine.
- Patients should be instructed to inform their health care provider if they develop any unusual symptom, or if any known symptom persists or worsens.
- Patients should be instructed to inform their health care provider of any other medications they are currently taking, including over-the-counter medications.
Indications
Dosing (Adult)
General Notes: Administer IV infusion over 60 minutes. Do not add additives or other medications to single-use vials or infuse simultaneously through the same IV line. If the same IV line is used for sequential infusion of additional medications, flush the line before and after infusion of therapy with appropriate infusion solution
Renal Dosing
Black Box Warnings
Warnings
Overdose
Drug Interactions
Special Populations
Breasfeeding
Chemical Structure
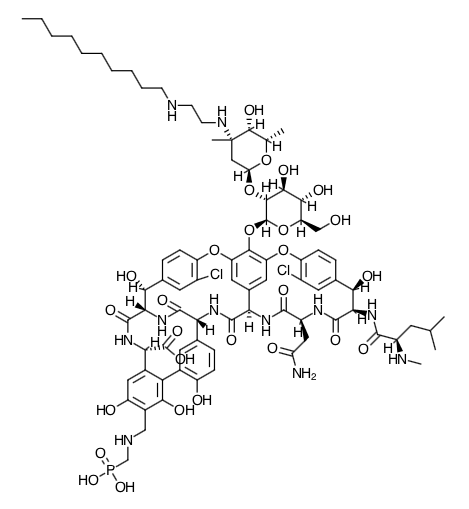
Pharmacodynamics
Pharmacokinetics
Counseling Points
MESH Terms & Keywords
|
|---|
|





