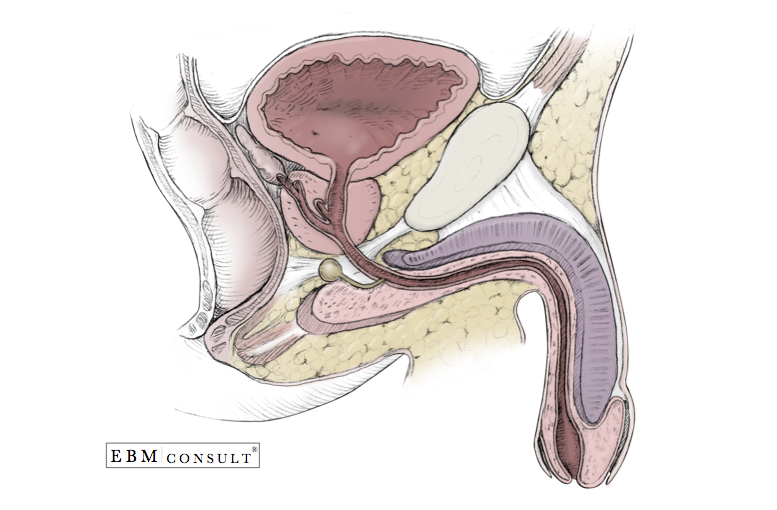
Male Genitourinary Anatomy - Urinary Bladder, Prostate, & Penis
|
|---|
- Anatomy:
- Distensible, hollow viscus that is surrounded mainly
by the detrusor muscle
- In males the neck of the bladder these muscle fibers form the involuntary internal urethral sphincter
- By the age of 6 years, the bladder is located relatively free within the extraperitoneal subcutaneous fat tissue and begins to descend down into the lesser pelvis (when empty), lying superior and posterior to the pubic bones of the pelvis
- Prior to the age of 6 years it sits in the abdomen
- When the bladder is full is ascends up into the greater pelvis and marked distension can go up into the abdomen
- Only the superior surface is covered by peritoneum
- In males - this separate from the rectum by the fascial rectovesical sputum and lateral by the seminal vesicles
- In females - it lies just superior and anterior to the wall of vagina
- The neck of the bladder is held firmly in place by the lateral ligaments of the bladder and tendinous arch of the pelvic fascia:
- In males the anterior portion is anchored by the puboprostatic ligament
- In females the anterior portion is anchored by the pubovesical ligament
- Function:
- Receives urine from the kidneys via the ureters
- Serves as a temporary reservoir for urine
- Blood Supply:
- Arterial supply: Branches of the internal iliac arteries
- Anterosuperior aspect is supplied by the superior vesical arteries
- Posteriorinferior aspect is supplied by:
- In males - inferior vesicle arteries
- In females - vaginal arteries
- Other parts of the bladder, supplied by branches from the obturator and inferior gluteal arteries
- Venous drainage:
- In males - the vesical venous plexus and prostatic venous plexus
- In females - uterovaginal venous plexus
- Lymphatic drainage:
- Superiorlateral aspect drains into the external iliac lymph nodes
- Fundus and the neck drain into the internal iliac lymph nodes and a small number will drain into the sacral lymph nodes
- Innervation:
- Presynaptic sympathetic nerve fibers from the T11 - L2/3 spinal cord level
- Presynaptic parasympathetic nerve fibers from S2-S4 spinal level and synapse with postsynaptic neurons in the bladder wall
- Anatomy:
- Also called Cowper glands
- Two pea size glands that lie posterolateral to the intermediate part of the urethra
- Function:
- Produce mucous secretions during sexual arousal that pass into the urethra
- Anatomy:
- In males the fibers of the detrusor muscle extend down to this area to form this sphincter.
- Function:
- Contracts during ejaculation to prevent ejaculate from entering into the bladder
- Anatomy:
- Composed of 3 cylindrical contractile bodies of erectile tissue that are surrounded by deep fascia (also called Buck fascia):
- Two Corpus Cavernosa located dorsally and covered and held together by the tunica albuginea
- One Corpus Spongiosum located ventrally and contains the spongy urethra
- The distal portion is the glans penis
- If uncircumcised, then the prepuce (extra skin) would be over this area
- Function:
- Provides outlet for urine and semen
- Blood Supply:
- Arterial supply: branches of the internal pudendal arteries
- Venous drainage: blood from the cavernous bodies drain by the venous plexus into the deep dorsal vein of the penis. The superficial parts drain into the superficial external pudendal vein.
- Lymphatic drainage: The skin of the penis drains into the superficial inguinal lymph nodes, where as the glans and distal spongy urethra drain into the deep inguinal lymph nodes and the cavernous bodies and proximal spongy urethra drain into the internal iliac nodes.
- Innervation:
- Primarily parasympathetic nerve fibers that are involved in erection
- Anatomy:
- Is normally about 3 cm long, 4 cm wide, and 2 cm in diameter and surrounds the prostatic urethra and is broken down into zones (peripheral and a central).
- 2/3 of made up of the glandular part and the other 1/3 is made up of the fibromuscular part
- The prostatic ducts open and empty to the posterior wall of the prostatic urethra
- Function:
- Produces a thin, milky white fluid that contributes up to 20% of the semen produced during ejaculation
- Blood Supply:
- Arterial supply: prostatic arteries, which are branches from the internal iliac artery, inferior vesicle arteries and a few from the internal pudendal and middle rectal arteries.
- Venous drainage: prostatic venous plexus
- Lymphatic drainage: internal iliac lymph nodes
- Innervation:
- Mainly sympathetic nerve fibers from levels of T12 - L2/3 spinal cord segments
- Anatomy:
- Lies between the fundus of the bladder and the rectum
- They do not store sperm
- Joins the ejaculatory duct
- Function:
- Secretes thick alkaline fluid with fructose (to serve as a source of energy for sperm) and a coagulating agent
- Blood Supply:
- Arterial supply: derived from the inferior vesicle and middle rectal arteries
- Venous drainage: accompany the arteries with similar names
- Lymphatic drainage: Both the internal and external iliac lymph nodes
- Anatomy:
- In males - 18 - 22 cm long
- Divided into 4 parts:
- Intramural (preprostatic) part
- Prostatic urethra
- Intermediate (membranous) part
- Spongy urethra
- In females - 4 cm long and 6 mm in diameter
- Function:
- In males - conveys urine from the internal urethral orifice to the external urethral orifice. It also provides an exit for semen, which contains sperm and prostatic secretions.
- Blood Supply:
- Arterial supply: in males, the proximal two parts are supplied by the prostatic branches of the inferior vesical and middle rectal arteries
- Venous drainage: prostatic venous plexus
- Lymphatic drainage: mainly into the internal iliac lymph nodes
- Innervation:
- Derived from the prostatic plexus and is a mixture of sympathetic, parasympathetic, and visceral afferent nerves.
Bladder
Bulbourethral Gland
Internal Urethral Sphincter
Penis
Prostate
Seminal Vesicle
Urethra