Fish
oil has been used to treat a number of conditions, which include asthma,
diabetes mellitus, rheumatoid arthritis, inflammatory bowel disease, systemic
lupus erythematosus, hyperlipidemia and cardiovascular disease (CVD).1-6 As
it relates to CVD, fish oil is most commonly used to treat high triglycerides
(hypertriglyceridemia). When clinicians refer to the use of "fish
oil", they are generally referring to omega-3 fatty acids (also known as
polyunsaturated fatty acids (PUFA)). These specific omega-3 fatty acids
include docosahexaenoic acid (DHA; 22:6n-3) and eicosapentaenoic acid (EPA;
22:5n-3).7 For the most part, neither DHA nor EPA cause any major side
effects or clinically relevant drug interactions, but they are known to
influence platelet function. As such, some clinicians perceive that this
can put the patient at greater risk of bleeding, especially during surgical
procedures or while on other medications that are known to affect coagulation
and platelet aggregation.
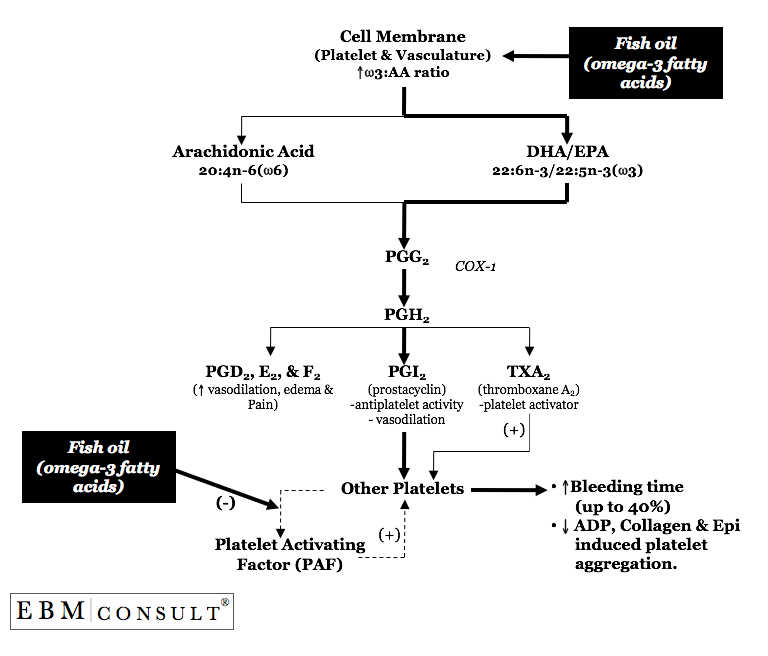
How
do omega-3 fatty acids affect platelet function and possibly increase the risk
for bleeding in certain situations?
After a platelet has been activated, a number of
intracellular reactions and changes take place to prepare the platelet for
binding during the formation of a primary hemostatic plug, and to help recruit
or activate other nearby platelets. One of these intracellular reactions
is the metabolism/utilization of cell membrane fatty acids to form various
eicosanoids, in particular thromboxane A2 (TXA2). It is well known
that TXA2 is a platelet activator and is used to facilitate platelet
aggregation. However, the type of membrane fatty acid
utilized can influence which metabolic pathway(s) within eicosanoid biochemical
synthesis predominates. In humans, one of the essential fatty acids
required and used in cell membranes is the omega-6 fatty acid, arachidonic acid
(AA). However, in patients who take fish oil supplements, the omega-3
fatty acids compete with AA for incorporation into the platelet cell membranes,
thereby increasing the ratio of omega-3 fatty acids:AA.8-10 This is
important because phospholipase A2 will then cleave more omega-3 fatty acids
from the cell membrane when needing to activate the ecosanoid intracellular
pathway. The omega-3 fatty acids (DHA and EPA) differ from AA in the
number of double bonds present and the location of the first double bond in
relation to the omega end of the fatty acid.7 Docosahexanoic acid has 6
double bonds and EPA has 5 double bonds, both with the first double bond
starting at carbon 3; whereas, AA has only 4 double bonds which start at carbon
6.7 Furthermore, both DHA and EPA are 22 carbons long whereas AA is 20
carbons long.7 This is the rationale for their respective names DHA
(22:6n-3), EPA (22:5n-3) and AA (20:4n-6).
Why
do these structural differences in fatty acids matter?
The various enzymes within the ecosanoid pathway have differential binding
affinities or preference for each of the types of fatty acids. As such,
when DHA and EPA are utilized the balance or preference is shifted towards a
greater degree of prostaglandin I2 production (also called PGI2or
prostacyclin) which has local vasodilatory and antiplatelet effects.11 In
addition, there is less formation of TXA2 which is known to activate
platelets.11 It is important to recognize that this process also occurs
within the vascular endothelial lining thereby creating an imbalance towards
the formation of antiplatelet ecosanoids (PGI2) versus TXA2.11 This shift
in the balance of ecosanoids is also a product of omega-3 fatty acids being
able to suppress platelet activating factor (PAF), a potent platelet activator.11,12
All of these effects translate to increases in bleeding time and a reduction in
ADP, collagen and epinephrine induced platelet aggregation in patients taking
omega-3 fatty acid supplements.9,10
Therefore,
it is biologically plausible that the use of fish oil supplements or
prescription omega-3 fatty acids could put certain patients at unwanted or
unnecessary risk for bleeding. However, in patients with underlying
cardiovascular disease and/or hypertriglyceridemia this biologic effect may be
beneficial. Part 2 of this series will answer the question of whether the
use of omega-3 fatty acids actually does cause more bleeding, especially in
surgical patients or patients taking an anticoagulant or antiplatelet agent.
References:
- Woods RK, Thien FC, Abramson MJ. Dietary marine fatty acids (fish
oil) for asthma in adults and children. Cochrane Database Syst Rev
2002;3:CD001283.
- Sirtori
CR, Crepaldi G, Manzato E et al. One-year treatment with ethyl esters
of n-3 fatty acids in patients with hypertriglyceridemia and glucose
intolerance: reduced triglyceridemia, total cholesterol, and increased
HDL-c without glycemic alterations. Atherosclerosis 1998;137:419-27.
- Kremer
JM, Bigauoette J, Michalek AV et al. Effects of manipulation of
dietary fatty acids on clinical manifestations of rheumatoid arthritis.
Lancet 1985;1:184-7.
- Belluzzi
A, Brignola C, Campieri M et al. Effect of an enteric-coated fish-oil
preparation on relapses in Crohn's disease. N Engl J Med
1996;334:1557-60.
- He
K, Song Y, Daviglus ML et al. Accumulated evidence on fish consumption
and coronary heart disease mortality: a meta-analysis of cohort
studies. Circulation 2004;109:2705-11.
- Bays HE. Safety considerations with omega-3 fatty acid therapy. Am J Cardiol 2007;99:35C-43C.
- Leiberman M, Marks AD, eds. Mark's Basic Medical Biochemistry A Clinical Approach. 3rd Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2009:479-566.
- Kim DN, Eastman A, Baker JE et al. Fish oil, atherogenesis, and thrombogenesis. Ann N Y Acad Sci 1995;748:474-80.
- Goodnight
SH Jr, Harris WS, Connor WE. The effects of dietary omega 3 fatty
acids on platelet composition and function in man: a prospective,
controlled study. Blood 1981;58:880-5.
- Lorenz
R, Spengler U, Fischer S et al. Platelet function, thromboxane
formation and blood pressure during supplementation of the Western diet
with cod liver oil. Circulation 1983;67:504-11.
- DeCaterina
R, Giannessi D, Mazzone A et al. Vascular prostacyclin is increased in
patients ingesting omega-3 polyunsaturated fatty acids before coronary
artery bypass graft surgery. Circulation 1990;82:428-38.
- Torrejon
C, Jung UJ, Deckelbaum RJ. N-3 fatty acids and cardiovascular
disease: actions and molecular mechanisms. Prostaglandins Leukot
Essent Fatty Acids 2007;77:319-26.






