There are 23.6 million children and adults
(7.8 percent of the population) in the United States alone that have diabetes
mellitus (DM).1 Unfortunately, 65 percent of the deaths in diabetic
patients are due to heart disease and stroke. In fact, adults with DM are
2 to 4 times more likely to have heart disease and/or a stroke than adults
without diabetes.2 The elevated cardiovascular risk in diabetics is
partially due to the high prevalence (about 73 percent of all diabetics) of
hypertension (defined as > 130/80 mm Hg) for which treatment with beta blockers
is indicated. 2 Thus, the use of beta blocking agents is relatively
common in those living with DM.
Beta
blockers, such as atenolol (Tenormin), metoprolol (Toprol; Toprol XL),
carvedilol (Coreg; Coreg CR) and many others, are known to be antagonists of
the noradrenergic response that results from the release of catecholamines by
the sympathetic nervous system.4-6 The sympathetic branch of the
autonomic system is activated primarily during an acute stress response
("fight or flight") and releases the predominant
neurotransmitter, norepinephrine, from post-ganglionic sympathetic nerve
fibers.7,8 In addition, the sympathetic nervous system also causes the
adrenal glands to release both epinephrine (80%) and norepinephrine
(20%). Norepinephrine and epinephrine may then activate the
adrenergic receptors of various organs, such as beta-1 receptors in the heart
which results in tachycardia (increase pulse).7,8 This acute stress
response can be activated by hypoglycemia (low blood sugar) which may occur
episodically in diabetic patients. Hypoglycemia generally occurs in
diabetics when the blood glucose level falls below 70 mg/dL and is most often
observed in patients receiving insulin or those being treated with tight
glucose control.8 During a hypoglycemic episode, most patients will
commonly experience tachycardia, tremors, shakes, and sweating that can serve
as a warning sign to the patient and encourage treatment with glucose.
As
mentioned previously, the use of beta-blockers in DM is common. Beta blocker
use is also very likely in this population since evidence suggests that
diabetic patients may receive greater cardioprotective benefits compared to
nondiabetic patients.9-11 However, many clinicians remain
reluctant to use beta blockers in those with DM because of concerns that these
drugs might block the effects of sympathetic (noradrenergic) activation that
occurs during hypoglycemic episodes. Therefore, these patients
might fail to recognize key symptoms of a hypoglycemic state and may neglect to
treat themselves appropriately.4-6
How can sweating be a possible sign of hypoglycemia while on a beta
blocker when sweating is also mediated by the sympathetic nervous system?
The autonomic nervous system is under subconscious control by sympathetic and
parasympathetic nerve cell bodies found in the medulla of the central nervous
system.7 In particular, catecholamines (norepinephrine and epinephrine)
are released by the following mechanisms from the sympathetic nervous
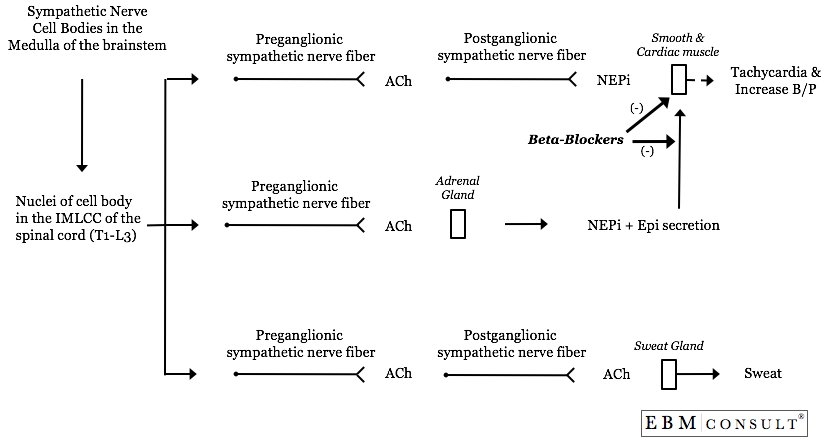
system. In the both mechanisms, sympathetic nerve cell bodies located in
the intermediolateral cell column (IMLCC) of the spinal cord (T1 - L3) have
preganglionic nerve axons that release acetylcholine in the sympathetic
ganglion that then activates nicotinic (or "ionotropic") receptors to
initiate an action potential on the postganglionic sympathetic nerve axon, or
directly acts on the adrenal gland to secrete epinephrine (80%) and
norepinephrine (20%) into the circulation.7 Outside of the adrenal
glands, in nearly all cases, the postganglionic sympathetic nerve fiber will
release norepinephrine at various target organs (such as smooth and cardiac
muscle) which can activate various adrenergic receptors (such as alpha-1,
alpha-2, beta-1, beta-2) needed for the acute stress response.7 While
this is true for most organs innervated by the sympathetic nervous system, it
is not the case for sweat glands. Instead, sympathetic postganglionic
nerve axons release acetylcholine, notnorepinephrine. The
released acetylcholine then activates nicotinic receptors (ionotropic) located
on the sweat glands, which are needed to help control body temperature that is
likely to increase during a fight-or-flight response. Therefore,
beta-blockers are not able to inhibit sweating, but can still inhibit
tachycardia and tremors, thus "masking" important signs and symptoms
that diabetic patients use to recognize hypoglycemic episodes.
Since
sweating during the activation of the sympathetic nervous system is mediated by
the release of acetylcholine via activation of a nicotinic receptor and not by norepinephrine
via an adrenergic receptor, diabetic patients taking beta blockers may only be
able to recognize sweating as a sign of a hypoglycemic episode. Due to a
number of variables, the exact percentage of diabetic patients experiencing
this problem is not known, but should be considered since untreated
hypoglycemia can be life-threatening.
References:
- American Diabetes Association. All About Diabetes. Accessed on 12/8/2009.
- American Diabetes Association.
- Hunt
SA et al. ACC/AHA 2005 Guideline update for the diagnosis and
management of chronic heart failure in the adult. A report of the
American College of Cardiology/American Heart Association Task Force on
Practice Guidelines (Writing Committee to Update the 2001 Guidelines for
the Evaluation and Management of Heart Failure. J Am Coll Cardiol
2005;46:e1-82.
- AstraZeneca LP. Tenormin (atenolol) product insert. Wilmington, DE. April 2003. Linked last accessed on 12/8/2008
- AstraZeneca
LP. Toprol XL (metoprolol succinate) product insert. Wilmington, DE.
July 2007. Linked last accessed on 12/8/2008
- GlaxoSmithKline.
Coreg CR (carvedilol phosphate) product insert. Research Triangle
Park, NC. April 2008. Last accessed on 12/8/2008
- Elfvin LG, Lindh B, Hokfelt T. The chemical neuroanatomy of sympathetic ganglia. Ann Rev Neurosci 1993;16:471-507.
- Zammitt NN,
Frier BM. Hypoglycemia in type 2 diabetes: pathophysiology, frequency,
and effects of different treatment modalities. Diabetes Care
2005;28:2948-61.
- Kjekshus
J, Gilpin E, Cali G et al. Diabetic patients and beta-blockers after
acute myocardial infarction. Eur Heart J 1990;11:43-50.
- Mykkanen
L, Kuusisto J, Pyorala K et al. Increased risk of
non-insulin-dependent diabetes mellitus in elderly hypertensive
subjects. J Hypertens 1994;12:1425-32.
- Cruickshank JM. Beta blockers continue to surprise us. Eur Heart J 2000;21:354-64.






